Minn. health care workers raise concerns about coronavirus response
Go Deeper.
Create an account or log in to save stories.
Like this?
Thanks for liking this story! We have added it to a list of your favorite stories.
Medical workers at hospitals across the Twin Cities are expressing concern that some health care facilities are not prepared to handle the expected surge of coronavirus patients.
The front-line workers are criticizing hospital administrators for slow implementation of strategies to treat coronavirus victims and unclear communication. They also say the hospitals are potentially putting medical workers at risk by rationing equipment and inconsistently enforcing protocols around coronavirus patients.
Minnesota hospitals say all efforts are being made to safeguard employees, obtain necessary equipment and prepare for the expected increase in infections.
While front-line staff acknowledged that hospitals are now preparing for some increase in infections, including taking the steps of identifying quarantine rooms where patients could be safely treated, most said their hospitals should have had concrete plans in place months ago.
Turn Up Your Support
MPR News helps you turn down the noise and build shared understanding. Turn up your support for this public resource and keep trusted journalism accessible to all.
“They knew this was coming. They should have been more prepared,” said Diana Carlson, a registered nurse in the intensive care unit at St. Joseph’s Hospital in St. Paul. “Once it started happening, it all of the sudden seemed to snowball and different departments got different memos, and nobody was talking to each other.”
Hospitals in the state have been working very hard in coordination with the Minnesota Department of Health and federal counterparts to prepare for the pandemic, said Dr. Rahul Koranne, president and CEO of the Minnesota Hospital Association.
“I would say that the hospitals and health care systems have been prepared for emergencies. We prepare for infectious outbreaks, we do a lot of drills, we prepare our front-line caregivers,” Koranne said. “We’re in a completely different situation right now, we’re in an emergent pandemic situation of unprecedented scale. It’s going to be impossible to prepare for a pandemic of this size.”
In nine interviews with MPR News since the weekend, front-line medical workers emphasized that communication about overall strategy was not filtering down to workers on the frontlines. Instead, nurses said they’re being asked to sort through sometimes contradictory advice from the Centers for Disease Control and Prevention and their own hospital’s protocols. They argued that front-line staff need speedy and thorough communications about hospital strategies, even if it’s daunting news.
“The guidelines have been all over the place and changing daily, while I understand that it's obviously a rapidly evolving situation, it affects those that are actually caring for the patients,” said Mary Forbes, a nurse at Abbott Northwestern Hospital in the intensive care unit. “They're just kind of all over the place, and that's not too reassuring as someone who's actually in the room with the patient for eight to 12 hours.”
Protocol for identifying possible coronavirus patients wasn’t always clear at some hospitals either, according to the medical workers. One nurse at a hospital in St. Paul who asked not to be identified because of concerns that talking publicly about the incident could endanger her job, described a patient who was treated for days for another condition that required fewer safety precautions before finally being tested for coronavirus. During that time, this nurse, and others, were possibly exposed to the patient. After asking, the nurse was told to self-monitor her conditions for at least the four days required to get the patient’s test results and given very little guidance.
Other front-line medical workers complained that protocols, such as limiting things like visitors, were not being clearly enforced. Forbes recalls clocking into work to find too many visitors in a patient’s room, in violation of current visitor policies.
“I'm supposed to keep track of visitors. I'm supposed to figure out what the right precautions are because I'm getting conflicting information from the CDC and from my hospital,” the nurse said.
Nurses at some hospitals said supplies were being rationed in a way that they thought threatened their safety, which they attributed to business practices that require hospitals to run “lean.”
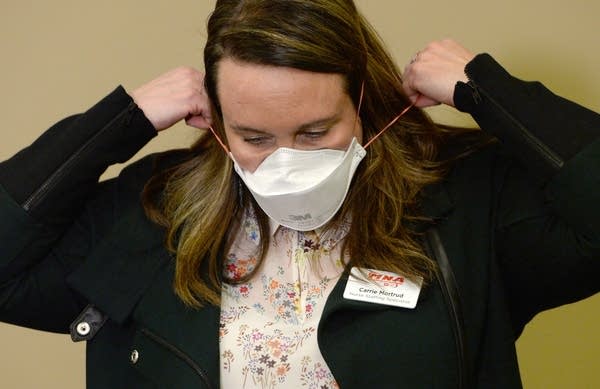
Medical staff also said they’re being asked to use surgical masks multiple times with possible coronavirus patients, which the Centers for Disease Control and Prevention guidelines acknowledge might be necessary. But front-line staff say reusing the masks over and over during the day can lead them to become moist from breath and potentially less effective at keeping out germs.
Communications sent by hospital officials confirm that reusing surgical masks, even with some suspected coronavirus patients, is current protocol at some hospitals. Other medical professionals cite limited access to what are called N95 masks, which prevent airborne contamination. The guidelines from the CDC have been controversial with the Minnesota Nurses Association and other groups.
“If you're sending me to take care of a patient that has an infection that is airborne, but you're instructing me to don the wrong precautions, I'm going to get infected,” said Cliff Willmeng, a nurse at United Hospital.
If medical professionals start to get sick, they said, the whole system will collapse. Some criticized policies for not requiring staff working with coronavirus patients to regularly check their temperatures, which other countries have required.
“If we're getting infected and we're being taken out of the rotation for caring for patients, all the while the volume and the acuity or the relative sickness of the patients is increasing,” Willmeng said. “We'll be overrun.”
Hospitals in the state are trying to figure out when supplies from the national strategic stockpile will start flowing into Minnesota, Koranne said.
Hospital systems have been making progress recently, according to many of those on the front lines. Staff described dramatically different situations surrounding protocol, equipment and communication at local hospitals, with a couple staffers applauding emergency preparations that have been made at their own hospitals.
Front-line workers said hospital administrators, like many in the public early on, may have fallen into the trap of wishful thinking about the pandemic.
“There was still this sort of assumption that we would only get a handful of cases that we could staff them one to one,” said St. Joseph’s Hospital nurse Melanie Timpano. “But today there is some acknowledgement that we need to be planning for what happens when our whole unit is COVID patients, or when we have a large number of them.”
Medical professionals are watching events in China and Italy with a sense of fear, said an emergency department nurse in Minneapolis, who asked not to be identified because of concerns about alienating colleagues at this time of crisis.
“It's kind of like a nightmare,” she said. “Looking around, some of my coworkers could die, or looking at my patients who are from a nursing home, these are the people who die. That's just incredibly sobering.”
Nurses, especially, described the trepidation with which they are approaching the coming months. Some said patients didn’t seem to understand how anxious and exhausted and scared they are too.
“I have to work regardless. So I’d rather feel like, ‘OK, I'm doing this because I want to help people rather than I’m doing this because I have to help people,” the nurse said. “I want to be a sanctuary for other people.”
Minnesota Hospital Association’s Koranne said it’s up to every person in Minnesota to take steps to ensure that there isn’t a surge in infections that overwhelms the state’s medical system and endangers medical workers.
“We are all in this together. The front-line caregiver, the health care team, the leaders, the state, the governor, we’re all in this together,” Koranne said. “We need every Minnesotan right now to make sure to stay at home, to practice social distancing, to not come into the clinic or the emergency department, but to call our providers.”
The Minnesota Nurses Association planned a news conference on Wednesday afternoon to air concerns members have about the health care system’s preparations.


