COVID-19 data gives reasons to be cautiously optimistic

Go Deeper.
Create an account or log in to save stories.
Like this?
Thanks for liking this story! We have added it to a list of your favorite stories.
Earlier this week the head of the World Health Organization expressed optimism that “the end is in sight” for the global COVID-19 pandemic, but he cautioned that “we are not there yet.”
This week’s COVID-19 data for Minnesota continues to show declines in cases, hospitalizations and some wastewater data. But deaths remain elevated, and the Metropolitan Council is reporting a 36 percent increase from the previous week in wastewater entering the Metro Plant for the week ending Sept. 12.
Michael Olsterholm, infectious disease specialist at the University of Minnesota, echoed the WHO’s balance of hope and realism in recent comments. Osterholm said “Let’s not fall victim to the allure of simply assuming the road ahead of us will be free of bumps or pothole. Minimizing [COVID-19’s] impact requires effort, it requires investment, it requires constant attention.”
The state of Minnesota seems to be following this advice. Gov. Tim Walz announced that additional free at-home tests will be available to Minnesotans from the state after the federal government suspended its program.
Turn Up Your Support
MPR News helps you turn down the noise and build shared understanding. Turn up your support for this public resource and keep trusted journalism accessible to all.
With that context in mind, let’s dig into what the data says about whether an end is in sight in Minnesota. And at the end of this week’s update, the latest from APM Research Lab on COVID mortality by race and ethnicity as well as vaccinations. And we look at how Minnesota compares to the rest of the country on these measures.
Cases and hospitalizations continue downward trend
Case rates are declining across all regions of Minnesota. Also of note is that case rates are fairly similar among the regions.

The next two graphs compare current hospitalizations and deaths with previous years. This time last year, hospitalizations were on the rise, associated with the increase in the prevalence of the delta variant. Two years ago, we were just on the brink of a rapid increase in hospitalizations.
Whether a fall-winter surge will occur this year is unknown, as it’s still a question whether or not COVID will be seasonal, like the flu.

Daily deaths are currently similar to the last two years at this time, but whether or not deaths will rise in the coming months, as they have before, is still unpredictable.

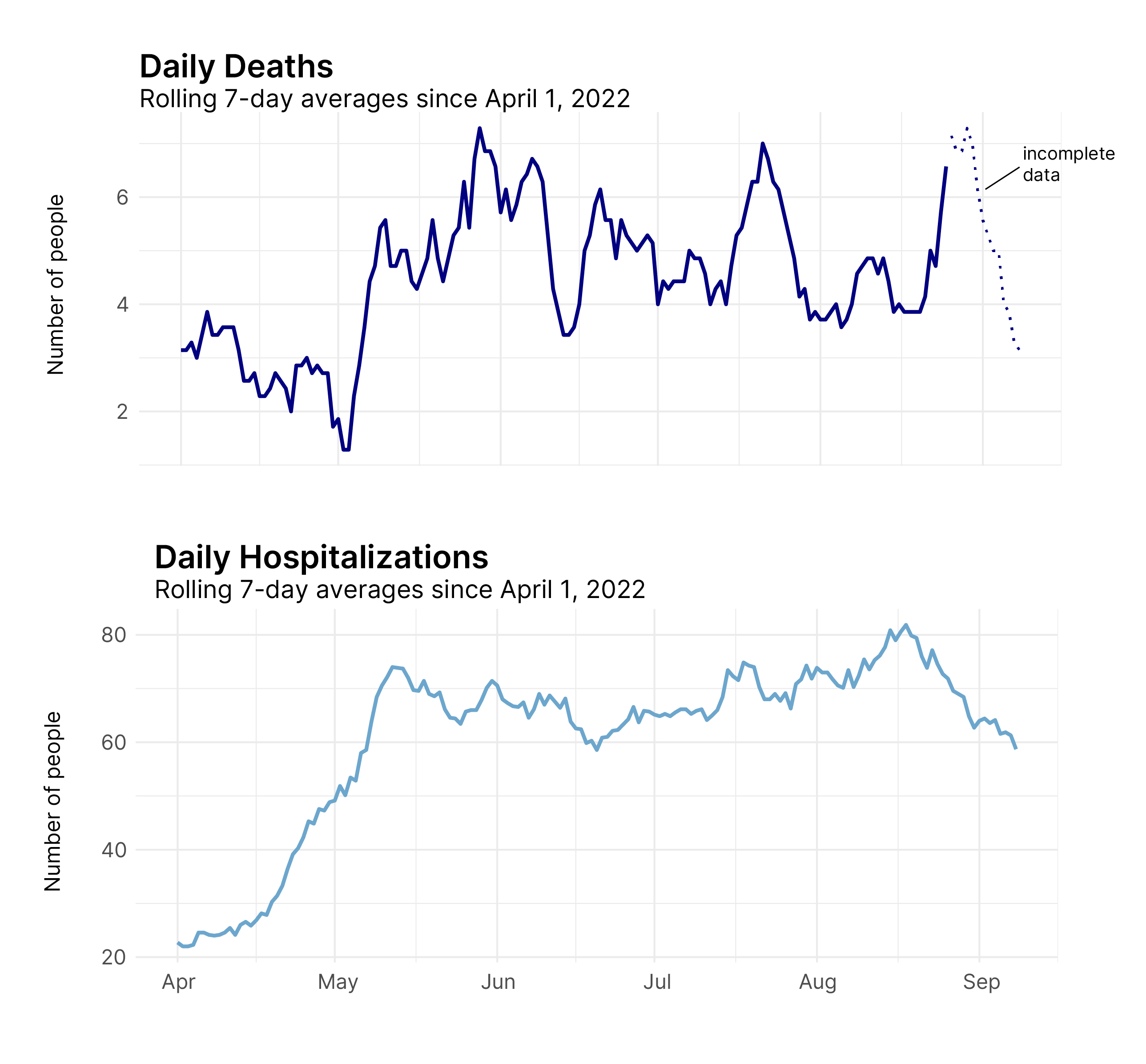
Since the yearly comparisons make it somewhat hard to distinguish the most recent data, here is a look at deaths and hospitalizations since last April. Increases in deaths seem to generally follow increases in hospitalizations, although the timing and extent to which that’s true varies. While death data is still coming in for recent weeks, it looks as though there will be a peak in late August, potentially surpassing any previous peaks this summer. But given that hospitalizations are on the decline, deaths should soon follow suit.
Wastewater shows recent increase in Twin Cities and new strain
The most recent wastewater analysis in the state, from the Metropolitan Council and the University of Minnesota’s Genomic Center, shows a 36 percent increase in COVID-19 levels entering the Metro Plant for the week ending Sept. 12. This reverses the falling levels over the previous two weeks and places us at back mid-August levels. Metropolitan Council staff say they “are not aware of any technical changes that could have influenced the Metro Plant load numbers this week.”
The increase could be a potential early indication that COVID-19 may not be declining as much as other metrics suggest. It is only one data point, however, and there can be short-term fluctuations that don’t impact the longer-term trends.

BA.5 continues to be the dominant strain of COVID-19 entering the Metro Plant. According to the Metropolitan Council’s summary: “BA.5 constituted 90 percent of the viral RNA entering Metro,” and BA.4 and BA.2 represented five percent and one percent, respectively. In a change from last week, BA.2.75 now constitutes one to two percent of Metro Plant influent; last week they tested for the new strain but did not detect it.
The latest data out of the University of Minnesota’s Wastewater SARS-CoV2 Surveillance Study, tracking data from seven regions through Sept. 4, shows a relatively positive picture. All regions, except the south central region, showed declines of COVID-19 levels over the previous four weeks and one week. The south central region saw a decline in the most recent week but a slight increase over the past month.
Fall may be around the corner, but Minnesota keeps looking green, according to the CDC
The map of Minnesota continues to be very green based on the Centers for Disease Control and Prevention’s latest weekly “Community Level” COVID-19 assessment, which rates 62 Minnesota counties low-risk. This is slightly down from the 67 low-risk counties rated by the CDC last week.
The good news is the CDC’s analysis puts only one Minnesota county in the high-risk category this week: Renville, in south-central Minnesota. That’s down from two high-risk counties last week. The CDC’s guidance for residents of high-risk counties includes masking up when in indoor public places.
A drop in both high-risk and low-risk counties means that the CDC rated more counties as medium risk than it did last week, mostly concentrated in the state’s north and south. However, the 24 medium-risk counties identified by the CDC this week is still half the number the CDC rated a few weeks, 51 for the week ending Aug. 25.
The CDC’s “Community Level” map accounts for both COVID-19 case rates and hospitalizations. Looking only at the latest weekly case rates, 55 of Minnesota’s 87 counties meet the CDC’s threshold for high transmission (100+ weekly cases per 100,000 residents), the same number as last week. Koochiching County has the state’s highest rate, with 262 officially reported cases per 100,000 for the week ending Sept. 14. Weekly case rates exceed 200 per 100,000 in four other counties in addition to Koochiching: Sibley, Mahnomen, Wadena and Renville.
On vaccines, Minnesota children are above average
In the last week, the APM Research Lab has published updates to its two ongoing coronavirus analyses — Inoculation Nation, which keeps track of COVID vaccine data, and Color of Coronavirus, which examines COVID mortality by race and ethnicity.
On the vaccine front, the number of doses administered has continually dropped for four months in a row. In August, 4.7 million doses were administered, down from 14.9 million in April. Those doses include booster shots — between April and August, at least 22 million U.S. residents received their second booster.
Those doses also include children’s vaccinations, which became available to children 6 months to 5 years old on June 18. As of Aug. 31, six percent of children under five have gotten at least one dose of the vaccine, and one percent of that cohort are considered fully vaccinated, equivalent to about 256,000 young children.
Children in Minnesota are vaccinated at about double the rate of the national average, with more than 12 percent of children under five having received at least one dose.

Nationally, COVID racial gap is narrowing, but not in Minnesota
Finally, our latest Color of Coronavirus this month includes a new section comparing mortality rates over time. One of our national analyses shows that Asian and Latino Americans have seen the biggest drop in COVID mortality rates compared to this point last year, with both groups having about half the rate this year compared to last year.
Notably, so far in 2022, white Americans have a higher crude COVID-19 mortality rate than any other major racial or ethnic group. In comparison, from January to July of 2021, Black, Pacific Islander and especially Indigenous Americans all had higher crude death rates than white Americans.
Critically, however, age-adjusted mortality rates show that racial disparities persist more than the crude rates might suggest. More on that in our full update.
Looking at recent hospitalizations in Minnesota reveals that even without age-adjustments, racial disparities exist between some groups that aren’t seen in this year’s national mortality data. In this summer’s COVID wave, for example, Black and Indigenous Minnesotans have seen the highest crude hospitalization rates.



